What does it mean to achieve worthy performance through instructional design for the workplace?
How do we measure the success of a course based on the level of performance achieved based on course objectives? Is it enough to develop content that fulfills the basic performance objectives without understanding the amount of behavioral change that we expect to occur after the learner completes the course?The challenge that we as instructional designers face is being able to develop sound content that measures the results of our performance objectives through tried-and-true methods of training evaluation, but also being able to take it one step further to determine whether the performance that we elicit through our instructional design is considered “worthy” performance.Worthy performance takes on special meaning when applied to the healthcare setting, because the inability to achieve it may adversely impact the quality of patient care. This is true for doctors, nurses, and healthcare specialists that have direct interaction with patients, as well as medical coders, billers, transcriptionists, and other professionals who do not have direct patient interaction, but who are responsible for maintaining quality and ensuring the accuracy of the medical record. Regardless of whether the learner has direct or indirect interaction with patients, the failure to achieve worthy performance can still affect the quality of patient care.
So what exactly is “worthy performance?”
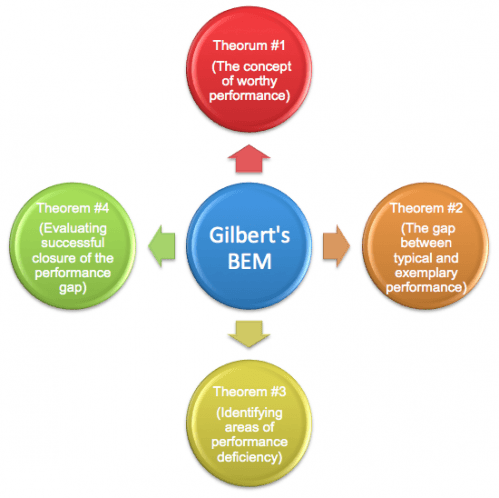
The concept of worthy performance originates from Thomas Gilbert’s Behavior Engineering Model (BEM). In his book, “Human Competence: Engineering Worthy Performance,” Gilbert addresses worthy performance within the framework of four leisurely theorems (leisurely being defined as the opportunity to improve upon something in relation to the time devoted to making the necessary improvements):
- Theorem #1 pertains to understanding the concept of worthy performance.
- Theorem #2 addresses the difference between typical and exemplary performance, and how to identify gaps between the two.
- Theorem #3 deals with identifying areas of performance deficiency and establishing methods of raising the standard of performance from typical to exemplary.
- Theorem #4 addresses how to evaluate accomplishments in relation to closing the performance gap.
 So with that being said, how can Gilbert’s Behavior Engineering Model be adapted to improve job performance for healthcare practitioners, as well as other learners outside of the healthcare arena?Follow these best practices to achieve worthy performance:
So with that being said, how can Gilbert’s Behavior Engineering Model be adapted to improve job performance for healthcare practitioners, as well as other learners outside of the healthcare arena?Follow these best practices to achieve worthy performance:
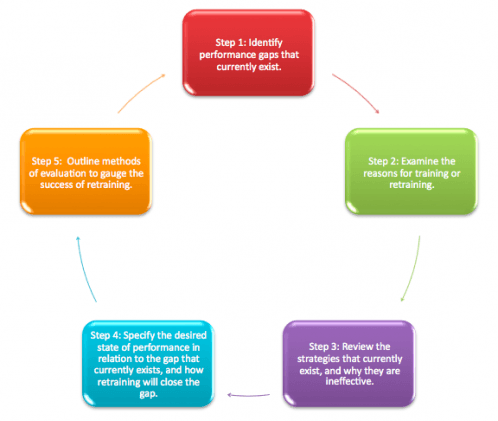
- Identify current performance gaps. Start by identifying gaps in performance, determining where performance deficiencies exist, and evaluating the impact of each deficiency in terms of the quality of patient care or the loss of healthcare revenue. Elicit learner feedback through anonymous questionnaires to determine where they feel performance gaps exist in relation to management performance expectations, and the training they feel that they need (or should have had but did not receive) to align their performance with management expectations.
- Examine the reasons for training or retraining. Based on the performance gaps that were identified in Step 1, examine the reasons that learners need to be retrained, and pinpoint deficiencies in the initial training that led to the need for retraining. Issues regarding diminished quality of patient care or medical recordkeeping should be addressed in the planning stages of curriculum development. If these issues are leading to a loss of healthcare revenue and are raising legal and ethical concerns due to lack of compliance, then these factors should also be addressed.
- Review the strategies for effective job performance that currently exist, and why they are not working effectively.Determine the current level of environmental support. Environmental support can include performance-related materials, tools, and rewards for exemplary performance. Review each practitioner’s repertoire of skills and behavior. Examine the level of knowledge that each healthcare practitioner has prior to retraining, their capacity for fulfilling performance expectations, and their level of motivation in terms of their desire to become exemplary performers.
- Specify the desired state of performance in relation to the gap that currently exists, and how retraining will close the gap. Based on the performance gap outlined in Step #1:
- Determine how retraining will close the existing performance gap.
- Outline what constitutes typical performance vs. exemplary performance based on the job description.
- Indicate how learners who are currently considered to be typical performers will become exemplary performers as a result of the retraining that takes place.
- Outline methods of evaluation to gauge the success of retraining, by asking these types of questions via a followup questionnaire three to six months following retraining:
- How did retraining close the existing performance gap?
- How did typical performance become exemplary performance as measured by the expectations outlined in the original job description?
- What changes have occurred from the learner’s perspective as a result of retraining?
- What changes have been witnessed from the standpoint of management in terms of quality and financial revenue?
Once retraining has taken place, and what was previously thought to be typical performance has become exemplary, or worthy, performance (as evidenced by the results of followup evaluation of both learners and management), worthy performance benchmarks can be incorporated into new training programs to eliminate training redundancy and to successfully meet the organization’s short- and long-term objectives for employee performance.Resources
Chyung, S. Y. (2008). Foundations of Instructional and Performance Technology. Amherst, MA: HRD Press, Inc, 106–113.











